He Opened His Eyes — But His Arm Wouldn’t Move*
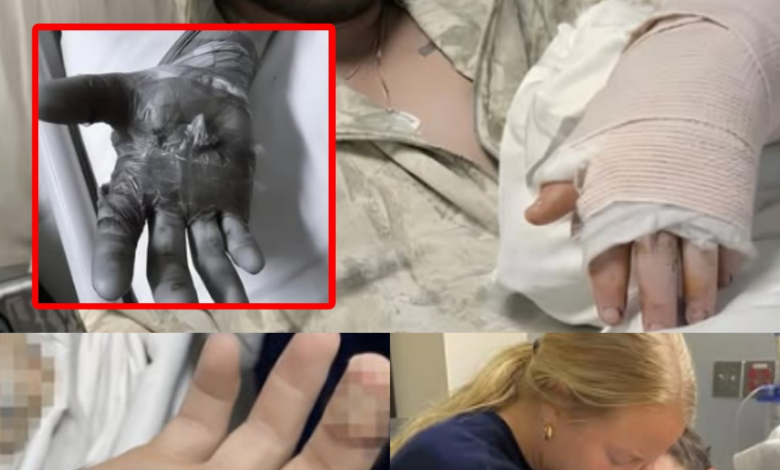
At 2:14 p.m., after hours in the operating room, Hunter opened his eyes.
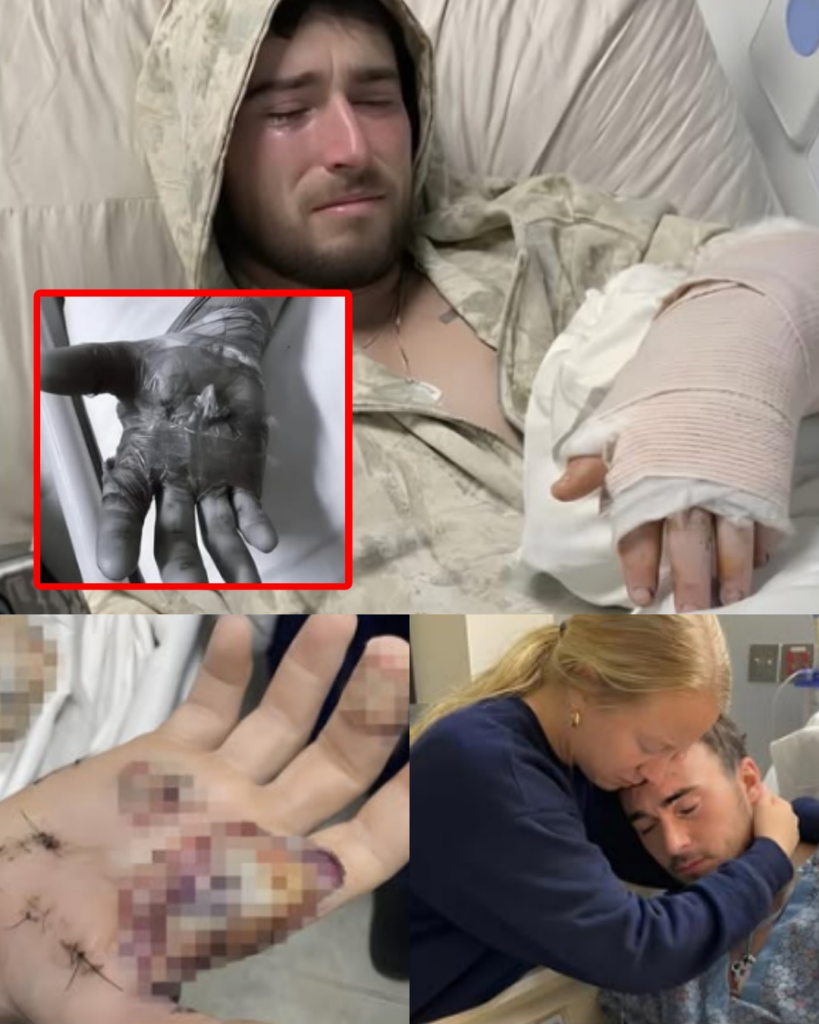
There was no cinematic gasp. No triumphant surge of relief. The fluorescent lights above him felt too bright. The air felt heavy. His body felt foreign — stitched, swollen, and exhausted from a battle it had barely survived.

For a moment, he didn’t remember where he was. Then the pain settled in, deep and radiating, not sharp but consuming. Machines hummed beside him. A monitor tracked the steady rhythm of his heartbeat. Somewhere nearby, a nurse quietly adjusted an IV line.
He turned his head slightly.
And then he looked at his left arm.
He tried to move it.
Nothing.
At first, he assumed the anesthesia hadn’t fully worn off. He focused harder. His fingers. His wrist. His elbow. He willed the muscles to respond the way they always had.
Still nothing.
The realization didn’t arrive dramatically. It crept in slowly — like cold water rising. He could see his arm. It was there, wrapped in thick dressings, elevated and secured carefully after multiple surgeries. But it did not feel like his arm anymore. It felt distant. Silent.
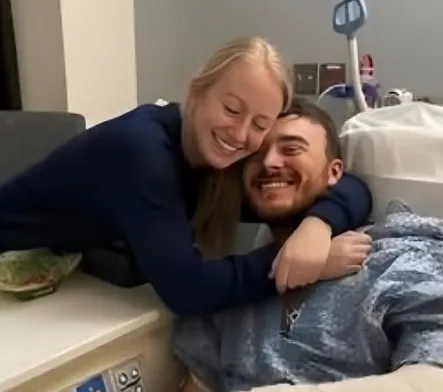
Doctors had prepared the family for this possibility. After catastrophic electrical trauma, the body reacts in complex and unpredictable ways. When thousands of volts pass through tissue, nerves can be stunned. Swelling can compress delicate pathways that carry signals from brain to limb. Muscles may survive, blood flow may be restored, infection may be prevented — and yet function can remain suspended.
The surgery, by every clinical measure, had been successful.
Bleeding was controlled. Damaged tissue was addressed. Infection risk was managed. Circulation was stabilized. The surgical team had done what medicine could do in the critical window that determines survival.
But survival is not the same as restoration.
Hunter blinked slowly, absorbing the weight of that truth without fully understanding it. His chest rose and fell steadily. His heart monitor traced each beat in reassuring green lines. He was alive.
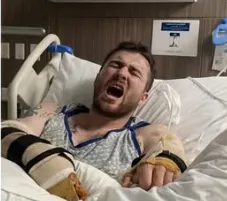
And yet, his arm would not move.
Across the bed, Katie never let go of his hand — his right hand, the one that still responded when she squeezed it. She had been there before he was wheeled into surgery. She had been there through every update, every hour of waiting, every quiet consultation outside swinging operating room doors.
Now she leaned close, her voice steady even if her eyes betrayed the exhaustion beneath.
“You’re here,” she whispered. “You’re still here.”
He swallowed, throat dry. The effort of speaking felt monumental. “My arm,” he managed.
The nurse, calm and practiced, explained what the doctors had already outlined: immobility can be common after trauma of this scale. Nerves can go quiet temporarily. Swelling can interrupt communication between brain and limb. The body, in crisis, prioritizes survival first. Function comes later — sometimes days later, sometimes weeks.
Sometimes longer.
It is a strange thing to survive something catastrophic. There is no instant reset. No immediate return to who you were. Instead, there is this in-between space — where life has been preserved, but certainty has not.
The hours that followed were not filled with drama. They were filled with waiting.
Neurological checks. Gentle prompts to try again. “Can you feel this?” “Can you wiggle your fingers?” Each attempt required energy he barely had. Each attempt ended in stillness.
But his heart kept beating.
And that mattered.
Doctors monitored swelling closely, adjusting medications to reduce inflammation around vulnerable nerve pathways. They explained that electrical injuries can create hidden damage — microscopic disruptions that imaging cannot always immediately reveal. Time, they said, would be a crucial diagnostic tool.
Time.
In crisis, everything happens at once. In recovery, nothing seems to move fast enough.
Katie stayed in her chair, fingers threaded through his. She spoke softly about ordinary things — the dog waiting at home, messages from friends, the sky outside the hospital window. Anchors to a world that continued moving even as theirs felt paused.
Hunter drifted in and out of sleep, each awakening bringing the same test. Look at the arm. Try to move it. Wait.
Nothing.
Yet beneath the silence in his limb, there was a different kind of motion — the quiet, relentless work of healing. Cells repairing. Swelling slowly receding. Nerves attempting to recalibrate after shock.
Rehabilitation specialists began outlining the next phase even before movement returned. Physical therapy. Electrical stimulation. Patience measured not in hours, but in months. Recovery would not be a straight line. There would be progress, setbacks, frustration.
Hope, too.
Because the absence of movement today does not always predict the absence of movement tomorrow.
That afternoon at 2:14 p.m., Hunter crossed a threshold. He moved from critical danger into uncertain recovery. The emergency had passed. The rebuilding had begun.
There is a quiet courage required in this space between surviving and restoring. It is not loud. It is not dramatic. It is measured in small attempts, in fingers that twitch weeks later, in muscles that remember how to respond.
His arm remained still.
But his heart did not.
And sometimes, in the fragile hours after catastrophe, that steady rhythm is the first promise that rebuilding is still possible.

