dq. Wall Suction Transition Signals Critical Stabilization in Hunter Alexander’s Right Arm Recovery
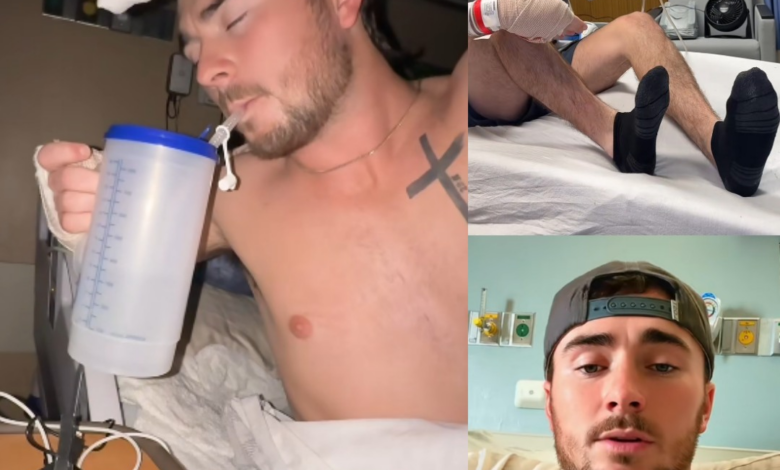
In the quiet choreography of hospital recovery rooms, progress is rarely dramatic. It does not arrive with applause or flashing lights. More often, it comes in technical adjustments — a setting lowered, a tube removed, a machine replaced. For Hunter Alexander, one of those subtle but significant changes has just taken place: the transition from a portable wound vacuum system to wall suction.
To most outside the medical world, it may sound like a minor equipment swap. To surgeons and critical care specialists, it signals something far more meaningful — stabilization.
Hunter’s right arm has been at the center of an intense medical battle. Following a severe injury that required complex surgical intervention, his care team implemented negative pressure wound therapy, commonly known as a wound vac. The device uses controlled suction to remove fluid, reduce swelling, improve circulation, and promote tissue healing. In critical cases, it also plays a key role in preventing infection — one of the most serious threats during early recovery.
For days, the steady hum of the portable suction unit was constant in his room — a reminder of both vulnerability and protection. It meant his wound required continuous active management. It meant the risk of fluid buildup or tissue instability remained high enough to demand vigilant oversight.
The shift to wall suction marks a turning point.
Unlike portable systems typically used in highly unstable or mobile cases, wall suction often indicates that a patient’s condition has stabilized enough for more standardized hospital support. It suggests that drainage levels are predictable, tissue response is improving, and the wound environment is controlled.

In simpler terms: his body is responding.
Medical professionals overseeing his care describe the transition as “encouraging and clinically appropriate.” The wound site has shown improved perfusion — meaning healthy blood flow is returning to the surrounding tissue. Swelling has decreased. Drainage output has become more consistent and manageable. Most importantly, there are no current signs of escalating infection.
That combination matters.
In upper limb trauma, especially involving the arm, circulation and infection control are paramount. The arm contains a complex network of nerves, blood vessels, and muscle groups that must function in coordination. Any prolonged instability can threaten long-term mobility and sensation.
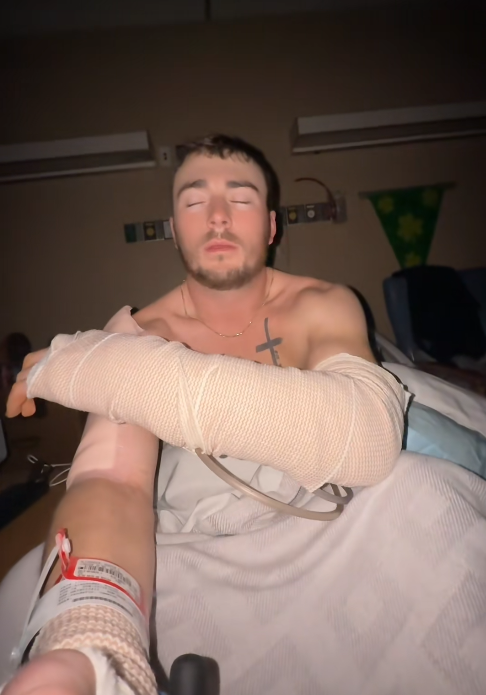
Hunter’s care team has been methodical. Regular imaging scans have monitored structural alignment. Lab work has tracked inflammatory markers. Dressing changes have been carefully timed to minimize disturbance while assessing healing progress. Each small improvement has built toward this moment.
The wall suction transition does not mean full recovery. It does not eliminate the possibility of further procedures or rehabilitation. But it does mean that the crisis phase is shifting.
Family members, who have remained at his side throughout the ordeal, describe the adjustment as “the first real exhale.” In a hospital environment where every beep can raise concern, quieter equipment and fewer urgent interventions feel monumental.
Rehabilitation specialists are already preparing for the next phase. With stabilization improving, attention gradually turns toward mobility preservation. Gentle range-of-motion exercises may begin soon under close supervision. Maintaining flexibility in the joints and preventing muscle atrophy will be critical in preserving long-term function.
Pain management remains part of the equation. Trauma recovery is rarely comfortable, and nerve sensitivity in the arm can complicate early healing. However, doctors report that Hunter’s discomfort levels are manageable and trending downward — another encouraging sign that inflammation is subsiding.
Experts note that wound vac therapy transitions are often a decisive indicator in surgical recovery trajectories. Remaining on aggressive suction for extended periods can signal complications. Moving toward standard wall support typically reflects improved structural integrity and wound stability.
In Hunter’s case, the timing aligns with other positive benchmarks. Vital signs remain steady. Laboratory indicators show decreasing systemic stress. Nutritional intake has improved, supporting tissue repair. Even small increases in energy levels have been noted by nursing staff.
Emotionally, stabilization brings a different kind of challenge. When a patient moves out of immediate danger, adrenaline fades. The long road of rehabilitation becomes clearer. It is a shift from survival to rebuilding — from crisis response to endurance.
For Hunter, that journey is just beginning.
Doctors caution that patience will be essential. Scar tissue formation, nerve responsiveness, and muscular strength will all require time and targeted therapy. Recovery of full function, if achievable, will depend on continued progress over weeks and months.
Still, the significance of this moment should not be understated.
In complex arm injuries, setbacks can occur quickly. Infections can spread. Circulation can falter. Tissue viability can decline. The fact that none of those outcomes are currently unfolding speaks volumes about the effectiveness of the treatment plan — and about Hunter’s resilience.
The steady hum of wall suction may not sound heroic. It may not draw headlines beyond those following his story closely. But within the sterile walls of a recovery unit, it represents something powerful: control restored, risk reduced, healing underway.
For now, that is enough.
The crisis phase appears to be receding. Stabilization is no longer just a hope — it is visible in clinical decisions and measurable improvements. And with each adjustment, each quieter machine, each steadier reading, Hunter Alexander moves one careful step closer to reclaiming the strength in his right arm.
Recovery remains a marathon.
But today, it has momentum.


