dq. Stabilization Surgery and Regenerative Treatment Mark Turning Point in Hunter’s Condition
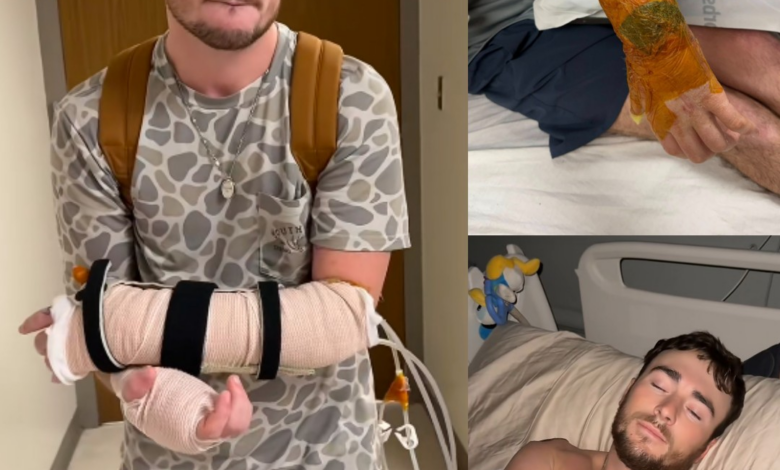
For weeks, the updates surrounding Hunter’s condition carried a tone of uncertainty. Doctors used careful language — “guarded,” “closely monitored,” “critical but stable.” Family members learned to measure hope in small increments: a steady heart rhythm, a reduced fever, a night without complications.
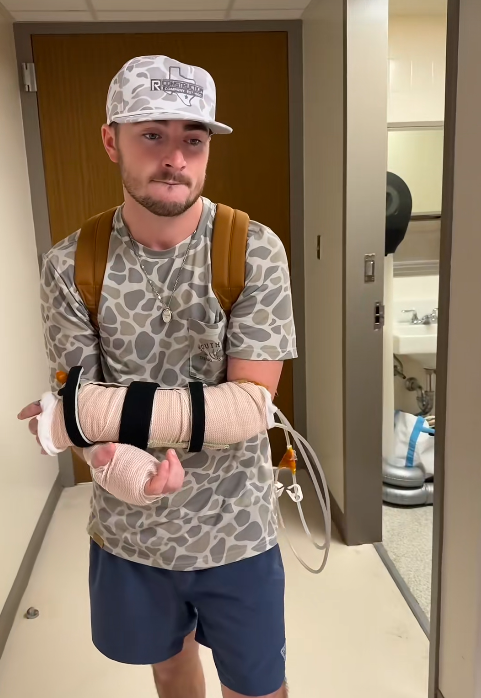
Now, for the first time since the ordeal began, there is a measurable shift in the narrative.
A complex stabilization surgery, followed by an advanced regenerative treatment protocol, is being described by medical staff as a pivotal turning point in Hunter’s recovery.
The procedure, performed by a multidisciplinary team of surgeons and trauma specialists, focused on reinforcing structural damage that had left Hunter vulnerable to cascading complications. According to sources close to the medical team, the surgery was not about dramatic reconstruction but about restoring balance — stabilizing compromised areas to prevent further deterioration.
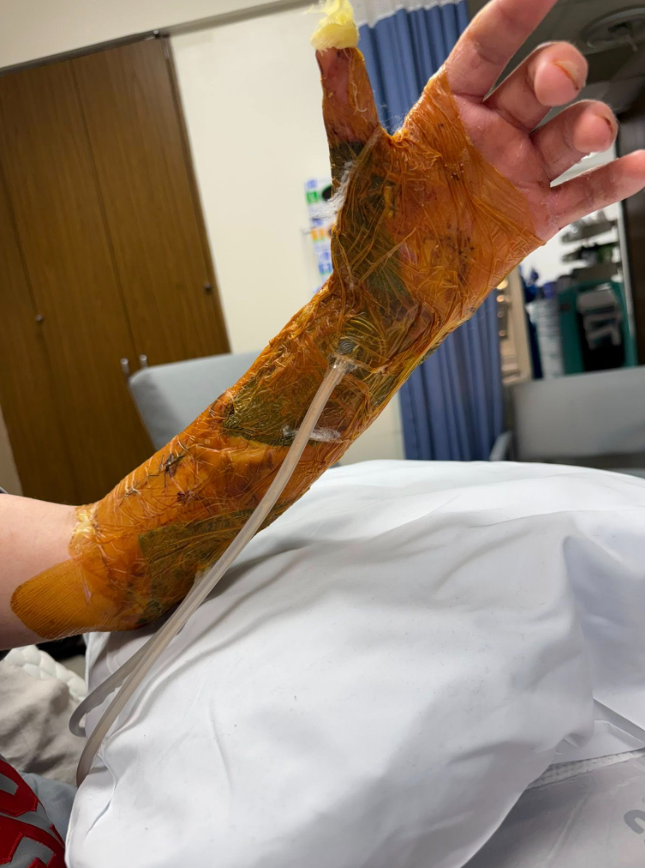
“It wasn’t a single fix,” one medical professional familiar with the case explained. “It was about creating conditions where healing could actually happen.”
Stabilization surgery often represents a critical crossroads in severe medical cases. Before it, the body is fighting to maintain equilibrium. After it, if successful, the body can begin the slower, more deliberate process of repair.
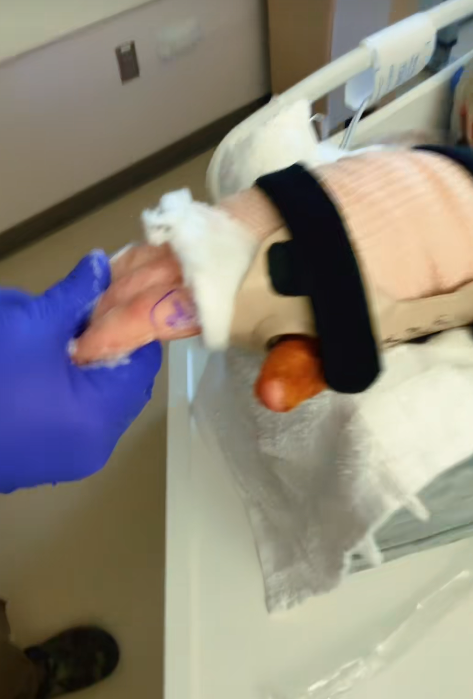
In Hunter’s case, that repair is being supported by regenerative treatment — an emerging field of medicine that aims to stimulate the body’s own healing mechanisms. While details remain private, regenerative therapies can include biologic injections, tissue-support matrices, or cell-based interventions designed to accelerate recovery and reduce inflammation.
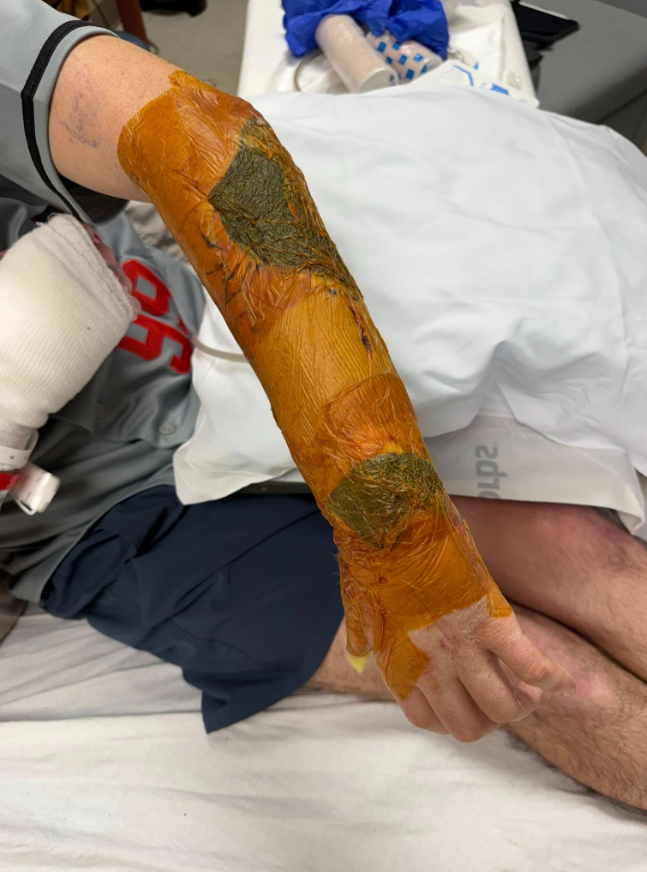
For families navigating complex trauma or post-surgical recovery, these treatments can offer something invaluable: time.
Time for tissue to mend.
Time for strength to return.
Time for hope to re-enter the room.
The days leading up to the surgery were tense. Physicians had observed that despite intensive care measures, Hunter’s progress had plateaued. Vital signs were holding, but not improving. Internal stress markers suggested that without intervention, setbacks could escalate quickly.
The decision to operate was not made lightly.
High-risk stabilization procedures require weighing potential benefit against significant strain on an already fragile system. But ultimately, doctors concluded that inaction posed the greater threat.
The surgery lasted several hours. Family members waited in silence, clinging to periodic updates delivered in measured tones. When the lead surgeon finally emerged, the message was cautiously optimistic: the procedure had achieved its immediate goals.
What followed, however, may prove just as significant.
Within 48 hours of the operation, subtle but meaningful improvements began to surface. Inflammatory indicators declined. Oxygen efficiency improved. Monitoring equipment reflected fewer fluctuations. While Hunter remains under close observation, the tone of medical briefings has shifted from crisis management to strategic recovery.
“It’s still early,” one clinician emphasized. “But this is the first time we can say we’re building forward instead of just holding the line.”
Regenerative medicine, though still evolving, has gained traction in recent years for its potential to enhance recovery after severe injury or surgery. Rather than simply repairing damage, these treatments aim to activate biological pathways that promote tissue regeneration and functional restoration.
Experts caution that outcomes vary widely depending on patient condition, timing, and underlying health factors. Still, in cases where conventional approaches reach their limits, regenerative therapies can offer a critical boost.
For Hunter’s family, the shift is emotional as much as medical.
Where once conversations revolved around risk percentages and emergency contingencies, they now center on rehabilitation timelines and incremental goals. Physical therapy planning has begun. Nutritional support strategies are being recalibrated to aid tissue repair. Even small milestones — longer periods of wakefulness, stronger grip responses — carry amplified meaning.
The road ahead remains long.
Stabilization does not guarantee full recovery. Regenerative treatment is not a miracle cure. There will likely be setbacks, difficult days, and careful reassessments. But the trajectory has changed.
And in critical care, trajectory matters.
Medical analysts observing the case note that turning points often arrive quietly. There is rarely a dramatic moment where everything shifts. Instead, improvement appears in data trends, lab results, and patient responsiveness — numbers and observations that, taken together, tell a new story.
That story is now cautiously hopeful.
Hospital staff describe a subtle change in atmosphere around Hunter’s room. The urgency that once defined every movement has softened into focused determination. Care teams are no longer bracing for collapse; they are planning for progression.
Family members, while protective of privacy, have expressed deep gratitude for the surgical team and specialists overseeing regenerative therapy. In a brief statement, they acknowledged that while challenges remain, they are encouraged by “the steady and meaningful progress we are finally beginning to see.”
For anyone who has waited beside a hospital bed, watching monitors flicker through long nights, this moment is familiar: not triumph, not certainty — but relief.
Stabilization surgery created a foundation.
Regenerative treatment is building upon it.
And for the first time since this ordeal began, Hunter’s condition is no longer defined solely by survival — but by the possibility of recovery.

