d+ Out of the ICU: Hunter Alexander’s Transfer Marks a Measured but Meaningful Turn in His Recovery
The hallway was quieter than usual.
No urgent footsteps. No alarms echoing off sterile walls. Just the soft hum of hospital wheels rolling forward — and with them, a shift no one dared to celebrate too loudly. After an extended and critical stay under constant medical supervision, Hunter Alexander has officially been transferred out of the intensive care unit.
It is not a declaration of victory. Not yet. But it is movement. And in medicine, movement matters.
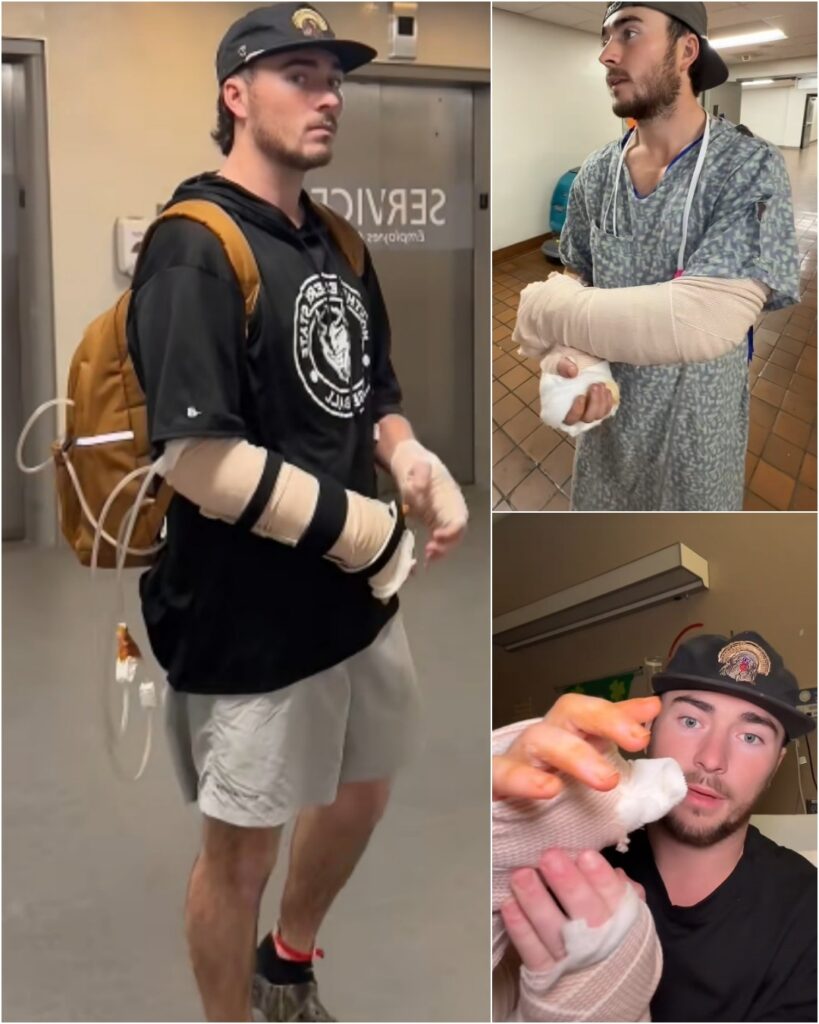
For days — stretching into what felt like an eternity for those closest to him — Hunter remained in the ICU, where time behaves differently. There, progress is measured in numbers glowing on monitors. In millimeters of improvement. In breaths that come a little easier than the one before. Every hour required vigilance. Every fluctuation demanded immediate attention.
Now, according to medical staff overseeing his care, Hunter’s condition has stabilized. His vital signs have remained within safe parameters, offering the first sustained period of physiological consistency since his admission. In critical care, stability is not a small word. It is earned.
Doctors also confirmed that a recent dressing change — a procedure that may sound routine but carries significant risk in fragile patients — was completed successfully and without complications. For families unfamiliar with the language of hospitals, it might seem like a minor clinical detail. For professionals and loved ones alike, it represents something far greater: resilience in the body’s ability to tolerate necessary interventions without spiraling backward.
The ICU is designed for constant intervention. Every patient there exists within reach of immediate life-saving measures. To be moved out is not symbolic. It is conditional — dependent on consistent signs that the body can sustain itself without minute-to-minute crisis management.
Sources within the care team describe Hunter’s transfer as cautious but appropriate. He no longer requires the same intensity of invasive monitoring. The machines that once dictated the rhythm of the room have quieted. The lighting is softer. The pace is slower. The next phase has begun.
Yet the shift from ICU to a step-down unit does not mean the road ahead is simple. Recovery, especially after a prolonged critical period, is rarely linear. Muscles weaken. Energy drains quickly. Even sitting upright can feel like an uphill climb. The body, having endured trauma and intervention, must relearn balance.
Medical professionals emphasize that the next 72 hours remain significant. Stability must hold. Infection risks must be continuously monitored. Wound healing must progress without setbacks. It is a phase defined less by emergency and more by endurance.
For Hunter’s family, the transfer carries a weight that cannot be captured in charts or medical notes. The ICU is a place where conversations are often whispered. Where every phone vibration sparks fear. Where hope and dread share the same chair in the waiting room.
To leave that space — even cautiously — changes the emotional atmosphere. There is room to breathe differently. Not fully relaxed. Not yet relieved. But steadier.
Hospital staff have remained measured in their tone. There are no grand predictions. No sweeping statements about timelines. Instead, there is careful language: “stable.” “Responding appropriately.” “Continuing to monitor.” In the world of recovery, these phrases carry more credibility than optimism ever could.
What makes this transition significant is not drama, but durability. Hunter’s vital signs have not merely improved for a few hours — they have remained consistent within safe parameters. That consistency is what allows physicians to reduce intensive oversight. It is what creates space for rehabilitation planning. It is what opens the possibility of forward motion.
The recent dressing change, completed without complication, also signals encouraging tissue response. In critical cases, wound management can be unpredictable. Swelling, infection, or unexpected bleeding can rapidly reverse progress. That none of those events occurred is not accidental; it reflects both medical precision and biological cooperation.
Recovery, however, is not measured solely in lab results. It is felt in small human moments: the ability to speak more clearly. The strength to lift a hand without assistance. The first time a nurse lowers the bed rails without immediate concern.
These moments do not trend on social media. They do not generate headlines. But they are the architecture of survival.
Hunter’s case remains under close observation. Physicians continue to evaluate his response to reduced monitoring and assess how his body adapts outside the intensive environment. Physical therapy consultations are expected as strength rebuilding becomes a priority. Nutrition plans are being adjusted to support healing. The transition phase demands coordination as much as vigilance.
For those following his journey, the move out of ICU offers something tangible. It is proof that the fight has shifted from crisis management to cautious rebuilding. That shift does not erase the severity of what came before. Instead, it acknowledges it — and moves forward anyway.
The coming days will determine how firmly this progress holds. Medicine is honest about uncertainty. But it is equally honest about milestones. And this is one.
No confetti. No declarations of triumph. Just a quieter hallway, a different room, and a patient whose body has steadied enough to take the next step.
In critical care, that is never small.
Hunter Alexander’s recovery is not defined by a single moment. It is being written hour by hour — in stabilized numbers, successful procedures, and a transfer that signals cautious confidence from the professionals guiding his care.
The ICU doors closed behind him. The journey continues ahead.
