d+ Hours, Not Weeks: Inside the Critical Surgical Window as Doctors Race to Protect Hunter’s Future.
The language changed first.
It wasn’t dramatic. No alarms blared. No frantic hallway sprints. Instead, it was a quiet shift in tone — the kind medical teams use when precision matters more than panic.
Time, doctors told the family, is no longer being measured in weeks.
It’s being measured in hours.
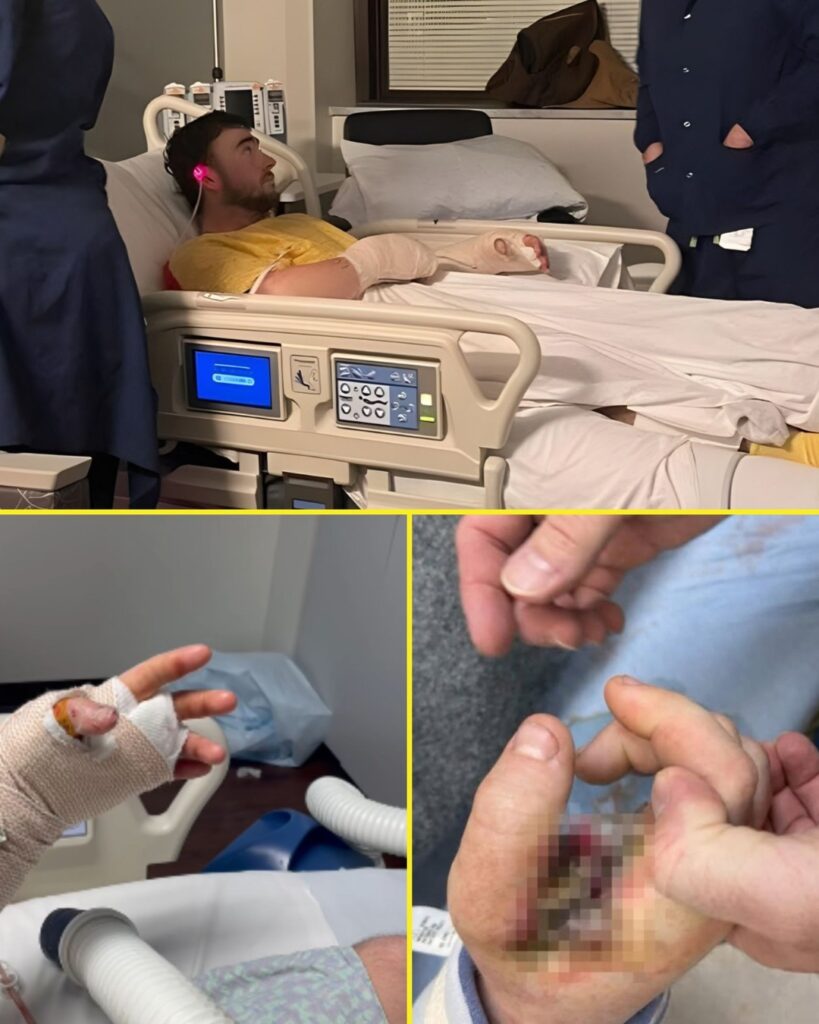
After days of intensive monitoring, specialists overseeing Hunter’s care have warned that he may require two to three additional surgical procedures in the coming days. The objective is urgent and unambiguous: preserve as much viable tissue as possible before the window narrows further.
In cases of complex electrical trauma, the visible injury is often only part of the story. Beneath the surface, tissue damage can continue evolving long after the initial event. Blood flow can shift. Swelling can intensify. Microscopic cellular injury can declare itself days later. What appears stable on Monday can deteriorate by Wednesday.
That unpredictable progression is why surgeons are moving deliberately — and quickly.
The Invisible Battle Beneath the Skin
Electrical injuries are uniquely deceptive. Unlike a clean laceration or a clearly defined fracture, high-voltage trauma can travel deep along nerves, muscles, and blood vessels. The current may enter in one place and exit in another, leaving behind a path of damage that does not always reveal itself immediately.
Specialists explain that tissue viability in these cases is not static. Compromised blood supply can lead to progressive cell death. Swelling within muscle compartments can increase pressure and further reduce circulation. Areas that initially seem salvageable can begin to show signs of necrosis as hours pass.
That is why Hunter remains under close observation.
His vital signs are being tracked hour by hour. Circulation is being evaluated repeatedly. Surgeons are assessing tissue color, temperature, responsiveness, and perfusion. Imaging studies and clinical examinations are being reviewed with meticulous care.
This phase of treatment is not dramatic in appearance. There are no headlines in the room. No speeches. Instead, there are measured discussions, calculated decisions, and contingency plans drafted in advance.
Each move is strategic.
The Surgical Tightrope
The dilemma facing the surgical team is as complex as it is consequential.
Remove too little damaged tissue, and infection or progressive necrosis can spread — potentially leading to systemic complications that threaten not just limb function but overall stability.
Remove too much, and the cost may be permanent loss of mobility, strength, or dexterity.
It is a surgical tightrope.
Doctors must determine margins — identifying precisely where healthy tissue ends and compromised tissue begins. In evolving electrical injuries, that boundary can blur. What is borderline today may declare itself clearly nonviable tomorrow.
That uncertainty is why multiple staged procedures are sometimes necessary. Rather than one aggressive operation, surgeons may return in phases — reassessing, removing newly demarcated tissue, and preserving as much function as possible with each pass.
Family members have been briefed carefully. They understand that two to three back-to-back procedures are not signs of failure. They are, in fact, often the best way to stay ahead of progressive damage.
Each surgery is an attempt to protect Hunter’s long-term future — not simply to stabilize the present.
Precision Over Panic
Despite the urgency, medical staff emphasize that urgency does not equal surrender.
The decision to move quickly reflects action — not desperation.
Every hour of monitoring informs the next decision. Specialists are watching for subtle shifts in circulation. They are evaluating swelling patterns. They are measuring laboratory markers that may indicate infection or muscle breakdown. They are weighing whether waiting another six hours could improve clarity — or cost opportunity.
Inside the hospital room, the atmosphere reflects that balance. There is tension, yes. But it is controlled tension. Conversations are steady. Plans are methodical.
Family members describe exhaustion — the kind that settles into the bones after consecutive sleepless nights. Yet they remain composed. They ask questions. They take notes. They prepare themselves for additional operating room doors closing and reopening.
They know that in complex trauma care, progress is rarely linear.
Community in the Quiet Hours
While medical teams work through surgical strategies, another force has quietly filled the room: community support.
Messages of encouragement continue to arrive daily. Friends, extended family, and even strangers have sent prayers and notes of strength. Those messages are read during long stretches of waiting. They have become part of the rhythm of the day — a reminder that this fight is not being carried alone.
In moments when hours feel heavier than days, that support matters.
Medical professionals often speak about the role of morale in recovery. While surgical skill and physiological resilience are critical, emotional endurance shapes the journey just as profoundly. Hope does not replace medicine, but it sustains those walking through it.
And for now, hope remains intact.
The Critical Window Ahead
The coming days will be pivotal — not because optimism is fading, but because precision now determines outcome later.
If viable tissue can be preserved, future rehabilitation becomes more promising. If circulation stabilizes and infection is prevented, long-term mobility may be protected. If surgical margins are chosen wisely, recovery pathways widen.
The stakes are high, but so is the focus.
Surgeons are preparing for possible additional procedures with detailed planning. Equipment is ready. Schedules are flexible. Teams are aligned. Each decision will be guided by real-time findings, not assumption.
In trauma medicine, there are moments when action must be immediate and forceful. There are also moments — like this one — when careful timing carries equal weight.
Hunter is in that second phase.
Hours matter. Observations matter. Millimeters matter.
But so does resolve.
The language may have shifted from weeks to hours, yet the underlying message remains steady: this is not the end of the fight. It is a critical chapter within it.
As doctors race to preserve what can still be saved, they are doing so with intention, expertise, and relentless focus. And as the hospital monitors continue their steady rhythm, one truth holds firm —
Urgency is not surrender.
It is strategy.
