d+ At 11 P.M., the Fight Turned Critical: Hunter’s Family Faces 24 Hours That Could Change Everything
At exactly 11 p.m., the tone inside Hunter’s hospital room changed.
What had been a cautious evening of monitoring and measured optimism shifted into urgent motion. Alarms sounded. Nurses moved quickly. Doctors spoke in short, precise sentences. Hunter had entered early-stage septic shock — a dangerous complication that can escalate rapidly if not contained.
Within minutes, his medical team made the call to switch him to the strongest intravenous antibiotics available. The new medications began flowing immediately, racing through his bloodstream in an effort to halt the infection before it could spread further. At the same time, specialists initiated continuous monitoring of blood flow to his fingertips — a detail that may seem small to outsiders, but one that now carries enormous weight.
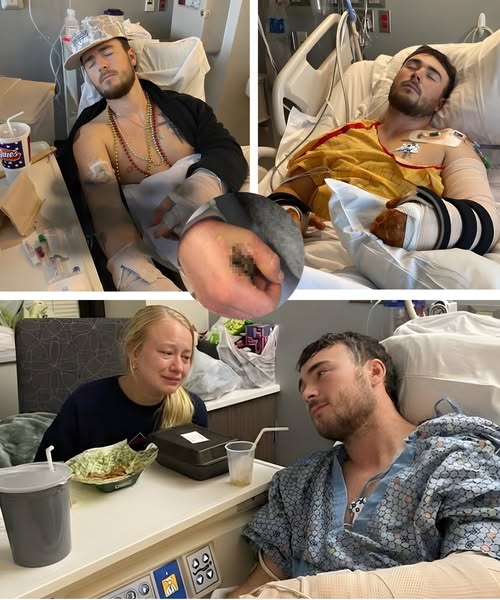
Because for Hunter, this fight is not only about surviving infection. It is about saving his hands.
“There are days when it feels like we take two steps forward… and then one step back,” Katie shared late last night, her exhaustion impossible to hide. Her words capture the emotional rhythm of the past several days — moments of real progress interrupted by sudden setbacks that threaten to undo it all.
Septic shock occurs when an infection triggers a chain reaction throughout the body, leading to dangerously low blood pressure and impaired circulation. In Hunter’s case, doctors are watching one critical indicator above all others: tissue viability in his hands. Reduced blood flow, even for a short period, can mean irreversible damage. Every hour matters.
Medical staff have confirmed that, for now, the tissue remains viable. That word — viable — is offering a fragile thread of hope. It means that despite the shock, despite the infection’s aggression, there is still circulation. There is still a chance.
But that chance is narrowing.
“The line between ‘saving his hands’ and ‘losing everything’ is very thin right now,” a member of the medical team explained. It’s a sentence no family ever wants to hear. It’s also the reality Hunter’s loved ones are facing as they prepare for what doctors are calling a critical 24-hour window.
In septic cases, the first day after intervention often determines the trajectory. If the antibiotics stabilize the infection and blood pressure holds steady, the body can begin to recover. If not, complications escalate quickly. That is why Hunter is now under constant observation. Monitors track his vitals continuously. Nurses assess circulation repeatedly. Every shift change includes detailed briefings. Nothing is left to chance.
Inside the waiting area, time moves differently.
Family members sit with phones in their hands but rarely look at them. Conversations trail off mid-sentence. Coffee goes cold. There is an unspoken understanding that any update could tilt the balance toward hope — or heartbreak.
Katie has barely slept.
Her exhaustion is not only physical but emotional. The past stretch of recovery had offered encouraging signs. Dressings were healing. Circulation appeared strong. Pain was manageable. There had been cautious optimism that the worst was behind them. Then, in a single late-night turn, the ground shifted again.
This is the cruel reality of severe infection recovery: progress is rarely linear. Families learn to celebrate small victories — stable vitals, improved lab numbers, a quiet night without alarms. But they also learn that setbacks can arrive without warning.
For Hunter, the battle now is intensely focused. Doctors are examining subtle changes: the warmth of his fingertips, the color of the skin, capillary refill time — how quickly blood returns after pressure is applied. These details may seem clinical, but they tell a life-altering story. They determine whether tissue survives or begins to deteriorate.
If circulation remains strong, further interventions may be avoided. If it falters, more aggressive measures could be necessary.
The next 24 hours will provide clarity.
Medical teams have emphasized that early intervention gives Hunter an advantage. The septic shock was caught in its early stage. Antibiotics were administered immediately. Monitoring began without delay. Those factors matter. They can mean the difference between containment and crisis.
Still, uncertainty hangs heavily in the air.
Outside the hospital walls, messages of support are pouring in. Friends, extended family, and even strangers who have followed Hunter’s journey are offering prayers and encouragement. In moments like this, community becomes a lifeline — a reminder that this fight is not being carried alone.
Katie says they are holding onto faith.
Not blind optimism. Not denial of the risk. But a steady, deliberate hope that the interventions now in place will hold. That the antibiotics will do their work. That the monitors will show improvement rather than decline. That when doctors step into the room for morning rounds, the news will lean toward relief instead of escalation.
Septic shock is formidable, but it is not unbeatable — especially when treated quickly. Hunter’s medical team is experienced and vigilant. Every variable that can be controlled is being controlled. Every sign of change is being addressed.
For now, the family waits.
They wait for lab results.
They wait for stable blood pressure readings.
They wait for the reassuring words: “He’s responding.”
And they wait with the understanding that this single day — these 24 fragile hours — may shape everything that comes next.
At 11 p.m., the fight intensified.
By this time tonight, they will know more.
Until then, Hunter remains under watch, surrounded by machines measuring every heartbeat, every breath, every pulse of blood reaching his fingertips. The battle between infection and intervention is unfolding quietly but decisively.
And somewhere inside that room, beyond the numbers and monitors, hope is still holding on.


