dq. BREAKING NEWS: Sudden Blood Vessel Erosion Sends Hunter Into Emergency ICU Lockdown — What Triggered This Dangerous Turn?
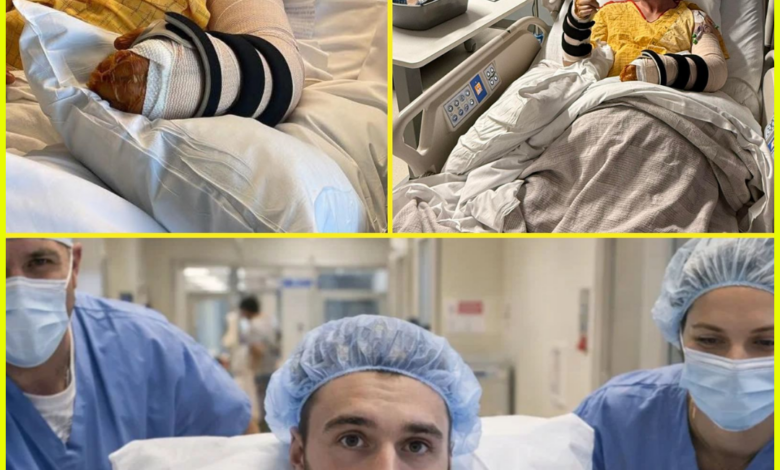
A sudden and alarming medical complication has placed Hunter back in critical care, as doctors confirm that unexpected blood vessel erosion triggered an emergency ICU lockdown late last night.

According to hospital sources familiar with the situation, Hunter had been showing cautious but steady signs of stabilization in recent days. Vital signs were reportedly holding. Surgical sites were being closely monitored. Physicians had described his condition as fragile, but not actively deteriorating.
That changed abruptly.
Medical staff identified signs of internal bleeding linked to erosion in a previously repaired blood vessel — a rare but serious complication that can occur following major trauma or complex surgical reconstruction. Within minutes, the intensive care unit shifted into emergency protocol.

Doors were secured. Additional surgical teams were alerted. Blood products were rushed in.
What exactly caused the erosion remains under investigation, but specialists explain that in high-risk recoveries — especially those involving electrical injuries, crush trauma, or multiple surgical interventions — blood vessels can become vulnerable. Tissue damage, infection risk, inflammation, and repeated procedures may weaken vessel walls over time.
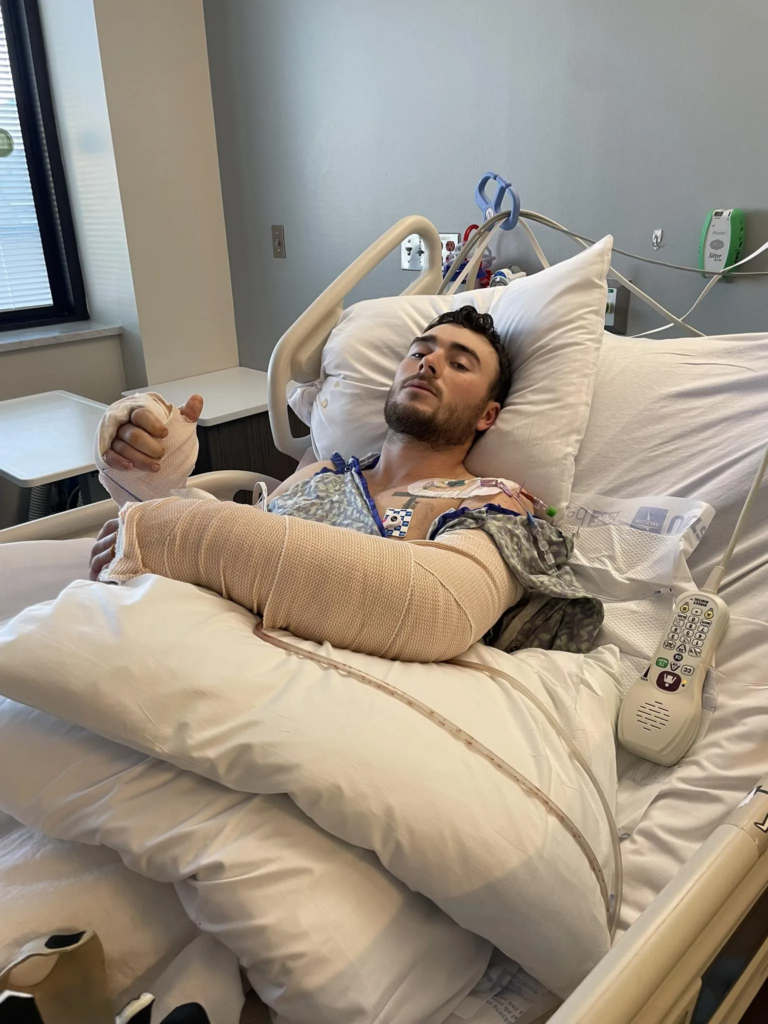
In some cases, erosion develops silently until bleeding begins.
Doctors acted swiftly. Hunter was stabilized and transferred under strict ICU containment measures to minimize movement and maintain constant monitoring. Ventilation support was reportedly adjusted, and vascular surgeons evaluated whether immediate operative repair was required.
Hospital officials have not released full details, citing patient privacy, but a source described the situation as “serious, but not hopeless.”
Understanding Blood Vessel Erosion
Blood vessel erosion occurs when the structural integrity of an artery or vein is compromised. This can result from infection, prolonged inflammation, surgical stress, or adjacent tissue breakdown. In post-trauma patients, especially those who have undergone grafts or vascular reconstruction, the risk is heightened.
When erosion occurs, it can lead to internal bleeding, clot formation, or sudden drops in blood pressure — all of which require rapid intervention.
Critical care experts note that early detection is key. Warning signs can include unexpected swelling, declining hemoglobin levels, localized pain, or changes in wound appearance. In ICU settings, frequent imaging and lab work help identify such complications before they escalate.
However, even with aggressive monitoring, sudden deterioration can happen.
Why the ICU Lockdown?
The term “ICU lockdown” does not necessarily imply a public safety threat. In medical contexts, it often refers to restricted access protocols during high-risk interventions. This allows physicians to control the environment, reduce infection exposure, and maintain uninterrupted focus during emergencies.
In Hunter’s case, the lockdown was reportedly implemented to manage both the vascular crisis and the potential for rapid systemic instability.
Critical patients experiencing internal bleeding may require rapid transfusions, emergency imaging, bedside surgical evaluation, or immediate transfer to an operating suite. Limiting foot traffic and external disruption is essential.
A Fragile Recovery Interrupted
Hunter’s journey has already been marked by multiple setbacks and incremental victories. Transitioning from acute trauma management into stabilization is often described as a delicate phase — one where the body is still vulnerable, even if outward signs appear calm.
Experts emphasize that recovery from severe injuries is rarely linear. Progress can plateau. Complications can emerge unexpectedly. What appears stable one day may shift dramatically the next.
“This is the nature of complex trauma,” one vascular specialist explained. “Healing tissue is fragile tissue. The body is rebuilding, but that rebuilding process has weak points.”
Family members have not released a public statement as of this writing, but sources close to them say they remain “deeply concerned but trusting the medical team.”
What Happens Next?
The immediate priority is controlling any active bleeding and reinforcing the compromised vessel. Depending on the extent of erosion, treatment options may include endovascular repair, surgical graft reinforcement, or localized clot stabilization.
If infection contributed to the erosion, antimicrobial therapy will likely be intensified. If pressure-related tissue breakdown is involved, adjustments in positioning and wound management may follow.
Doctors will also assess whether the incident affects Hunter’s broader recovery timeline. Extended ICU stays can impact mobility, muscle strength, and overall resilience, particularly in patients already recovering from major trauma.
Cautious Watchfulness
For now, Hunter remains under intensive observation. Physicians are expected to provide updated guidance once the immediate risk window passes.
Medical professionals stress that while this development is dangerous, rapid detection and intervention significantly improve survival odds. The coming hours will be critical in determining whether stabilization holds.
In severe recoveries, setbacks can feel devastating. But critical care teams are trained precisely for moments like this — when seconds matter and experience makes the difference.
Hunter’s condition remains serious.
But the fight is ongoing.

