d+ A Different Kind of Silence: Inside the ICU Morning That Gave Hunter’s Family a Fragile New Hope
SHREVEPORT, La. — Just before sunrise on Tuesday, the intensive care unit at LSU Health Shreveport felt different.
Not louder. Not calmer. Just… different.
There were no dramatic announcements, no sudden rush of footsteps, no triumphant smiles exchanged over hospital masks. Instead, there was a quiet shift — subtle enough that no one said it out loud at first, but powerful enough that everyone in the room felt it.
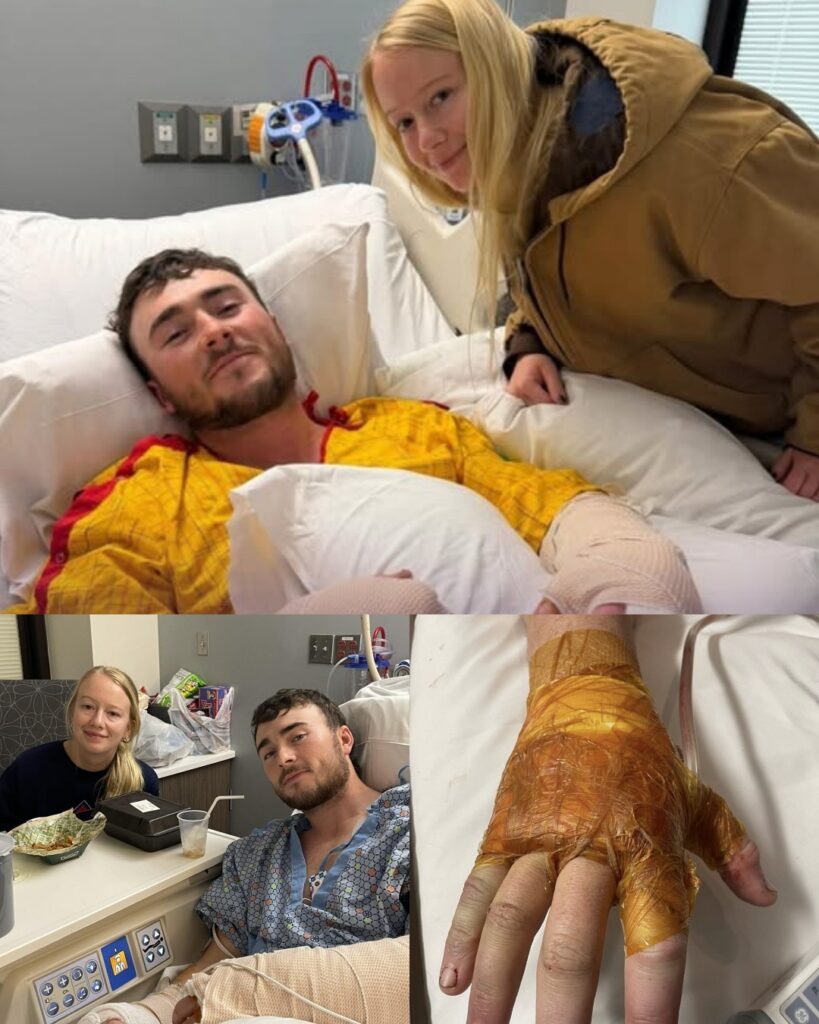
After everything his body has endured, Hunter showed signs — small, measured, but meaningful — of improvement.
In a battle defined by hours, sometimes even minutes, small can mean everything.
For weeks, Hunter’s recovery has been described in cautious terms: critical, complex, unpredictable. His injuries demanded constant vigilance. Machines hummed through sleepless nights. Nurses monitored vital signs in near darkness. Family members learned to read the language of beeping monitors and whispered medical updates.
Rest has been rare. Peace, even rarer.
But early Tuesday morning, something changed.
According to family members, Hunter slept through most of the night — an achievement that might seem ordinary outside hospital walls, but inside the ICU felt monumental. He woke around 4 a.m., a detail that his loved ones repeated quietly, as if afraid to disturb the fragile victory embedded in those few hours of uninterrupted rest.
Sleep, in critical recovery, is not just comfort. It is repair. It is recalibration. It is the body deciding, for a moment, not just to survive — but to stabilize.
Later that morning, medical staff carefully helped Hunter sit upright in a wheelchair while they worked through dressing changes on his right hand. The movement was controlled. Intentional. Closely supervised.
To an outsider, sitting up might not seem like a milestone. In this ICU room, it was.
“It may sound small,” one family member shared. “But in this fight, small is everything.”
The process was deliberate. Nurses adjusted lines and monitors. Circulation was assessed. Wounds were examined closely. The room carried that familiar ICU tension — focused but quiet — as clinicians evaluated how his body responded to even slight positional changes.
Because progress, with injuries like Hunter’s, is rarely linear.
Doctors are not celebrating yet.
Behind the scenes, labs are still being monitored carefully. Blood work is reviewed hour by hour. Circulation in injured areas remains under close evaluation. Every dressing change reveals critical information. Every data point contributes to the larger question: Is his body gaining ground — or simply holding the line?
That distinction matters.
Later today, one decision could determine where Hunter spends the next phase of his recovery. Will he remain in the ICU under full critical care monitoring? Could he transition to a step-down unit with slightly reduced intensity? Or does his body need more time within the highest level of hospital support?
The choice will not be symbolic. It will be clinical, data-driven, and deliberate.
A full medical update is expected to clarify what happened overnight and outline what comes next in the hours ahead. For Hunter’s family, those updates have become emotional checkpoints — moments where hope and caution coexist uneasily.
Because hope is present now. But it is cautious.
Medical experts emphasize that recoveries from severe trauma can pivot quickly. A strong morning can give way to a complicated afternoon. Stability can shift. Infection risks remain. Circulatory challenges demand vigilance. Even minor changes require immediate response.
That reality tempers any early celebration.
Still, those closest to Hunter describe Tuesday morning as carrying a different emotional weight.
There was no dramatic breakthrough. No single number on a monitor that triggered applause. Instead, there was the cumulative effect of subtle signs: sustained rest, responsiveness at dawn, tolerance for upright positioning, steady vital trends.
Sometimes recovery is not a leap forward. Sometimes it is the absence of a step backward.
For families in intensive care waiting rooms across the country, that nuance is deeply understood. Stabilization is a victory. Maintaining ground is progress. The body choosing to endure another day — on slightly steadier terms — can feel like a quiet triumph.
Inside Hunter’s ICU room, the atmosphere reflected that delicate balance.
Nurses continued their rounds. Physicians reviewed charts. Conversations remained measured. No one used the word “turnaround.” No one promised momentum.
But there was something unspoken in the air — a collective awareness that the morning did not feel like the previous ones.
The hours ahead will determine whether that feeling translates into sustained clinical progress. The potential move from ICU to step-down care is not merely logistical; it signals a shift in the intensity of monitoring, a recalibration of risk. Yet doctors are clear: decisions will be made based solely on medical readiness, not emotion.
As one clinician reportedly told the family, “We move when his body tells us it’s ready.”
For now, Hunter remains under close observation. Labs will continue to guide decisions. Circulation assessments will remain meticulous. Wound response will be tracked with precision.
The next 24 hours are critical.
But this morning — this quiet, unassuming morning — offered something that had been fragile for days: a sense that his body was not simply reacting, but responding.
Not dramatically. Not loudly.
Just enough to make everyone pause.
And sometimes, in the controlled chaos of an intensive care unit, that pause — that shared breath between fear and possibility — is enough to hold onto.


